

This article describes a peer support project developed and carried out by a group of experienced mental health professionals, organized to offer peer psychological support from overseas to healthcare professionals on the frontline of the COVID-19 outbreak in Wuhan, China. This pandemic extremely challenged the existing health care systems and caused severe mental distress to frontline healthcare workers. The authors describe the infrastructure of the team and a novel model of peer support and crisis intervention that utilized a popular social media application on smartphone. Such a model for intervention that can be used elsewhere in the face of current global pandemic, or future disaster response.
China was the first country hit by the COVID-19 pandemic. The currently known first reported case was recorded on Dec 8, 2019. It was not officially announced as a human-to-human transmitted disease by the Chinese government until Jan 20, 2020. Prior to that, many local physicians noticed a new kind of pneumonia caused by an unknown pathogen and Ai Fen, known as the “whistle distributor”, initiated the reporting procedure to the local contagious disease control agents. Other physicians, including the soon to be well-known whistle-blower, Dr. Li Wenliang, posted their concerns about SARS-like cases on WeChat, a Chinese social media and messaging application, but received administrative warnings and were summoned by local police. On Feb 7, 2020, Dr. Li WenLiang died from COVID-19 pneumonia. It has been reported that more than 3300 healthcare professionals contracted the Coronavirus while on duty, including at least 13 of them who lost their lives (https://www.businessinsider.com/healthcare-workers-getting-coronavirus-500-infected-2020-2). In addition, many more healthcare professionals have faced intense stressors leading to mental health crises.
Wuhan is the major transit hub of China. Two days before the traditional Chinese New Year Lunar Spring Festival on Jan 25 2020, when millions were traveling in the “biggest human migration on our planet,” the entire city with a population of 11 million was suddenly closed down. As a result of the lack of systematic crisis response infrastructure, information transparency, and clear guidelines, the remaining nine million people in Wuhan fell into a chaotic panic. Tens of thousands of people flooded into the local hospitals requiring acute health care and the local health system was overloaded to the edge of breakdown. Frontline health care workers faced this crisis with inadequate resources.
At this point, a group of Chinese speaking mental health professionals from the USA, Canada and Australia assembled a team to provide peer-to-peer psychological support for the Wuhan healthcare professionals who were fighting at the front line of this epidemic crisis. We recognized the urgent need to provide crisis psychological support and intervention for the frontline medical care providers. Hence this project was initiated immediately.
In consideration of the Chinese political environment and the safety of the front-line medical personnel in Wuhan, we maintained strict political neutrality and restricted or minimized sensitive political topics in our discussions. This was a grassroots independent project. We were not affiliated with any official or unofficial organization. We were aware of Chinese official licensure regulations and the possibility of being monitored by Tencent, a Chinese company who owns WeChat.
Below is a description of the challenge we faced in the early phase of the project:
It was a very different situation we were encountering, which can be imagined in the following way: You are running a group, and you know who signed on, but you don’t know who will come. When the time comes, you start the group with a blindfold covering your eyes. You can’t see if there’s anyone sitting in the room, nor you can hear anyone talking. You can’t reach anyone, but can only wait till someone in the group reaches out to you.
So you start the group. You know participants are suffering, anxious, angry, distressed and devastated, afraid. You want to build up a safe harbor for them, a place where they can feel safe and supported. You need to think about a way to engage your silent audience, as you know they are there (although you don’t know who) and you want to provide help.
You start to try different methods to engage them, such as playing some soothing music, talking about your life experience or previous relevant clinical situations, or giving tips about techniques for relaxing or sleep improvement. You also promise confidentiality and remind them gently that you are here to help and listen. Step by step, one by one, they reach out to you and talk to you in private, open up to you about their struggle, and you utilize your knowledge, experience, and heart to provide comfort. You get feedback from those with whom who you talked and much of the feedback is positive.
You feel somewhat overwhelmed about what you hear, which confirms some of the rumors circulating on various social medias which is not consistent with official news report. You appreciate that you have other teammates who support one another. You know it’s a long battle.
Crisis intervention is time-limited and therefore an exit plan or strategy should be in place. Connection with local mental health resources needs to be established for referrals, although the majority of the cases may not need long term follow up. There are two types of local referral sources, one is traditional local mental health agencies, and the other one is China-based mental health hotline.
Since this was a peer support service, it is not considered as “treatment” and thus protects professionals from being viewed as operating without proper licensure. We did not establish patient-professional relationships, we did not keep notes. This was strictly social support from a caring and concerned network. If clinical interventions are involved, then proper license would be required by different regulatory bodies.
This normally is not an issue when only crisis intervention of this type is involved, but we would recommend obtaining legal consult before starting such a service. If further clinical services are to be provided, malpractice insurance may be required.
Our group initiated this project out of a desire to help colleagues in Wuhan. There were no other interests involved, including political or monetary ones.
As Elisabeth Kübler-Ross described the seven-stages of emotional responses to acute stressful events resulting in grief and loss (https://en.wikipedia.org/wiki/K%C3%BCbler-Ross_model), we have encountered these similar stages among people in Wuhan in general and in our served medical staff. In addition, we have observed other changes that may be unique to this particular epidemic.
More effective procedures were put into place. With the growing number of recoveries, healthcare workers started to regain hope and confidence.
Our group started to intervene at Stage 3/4. By the end of this project most healthcare providers we were serving were in Stage 8/9.
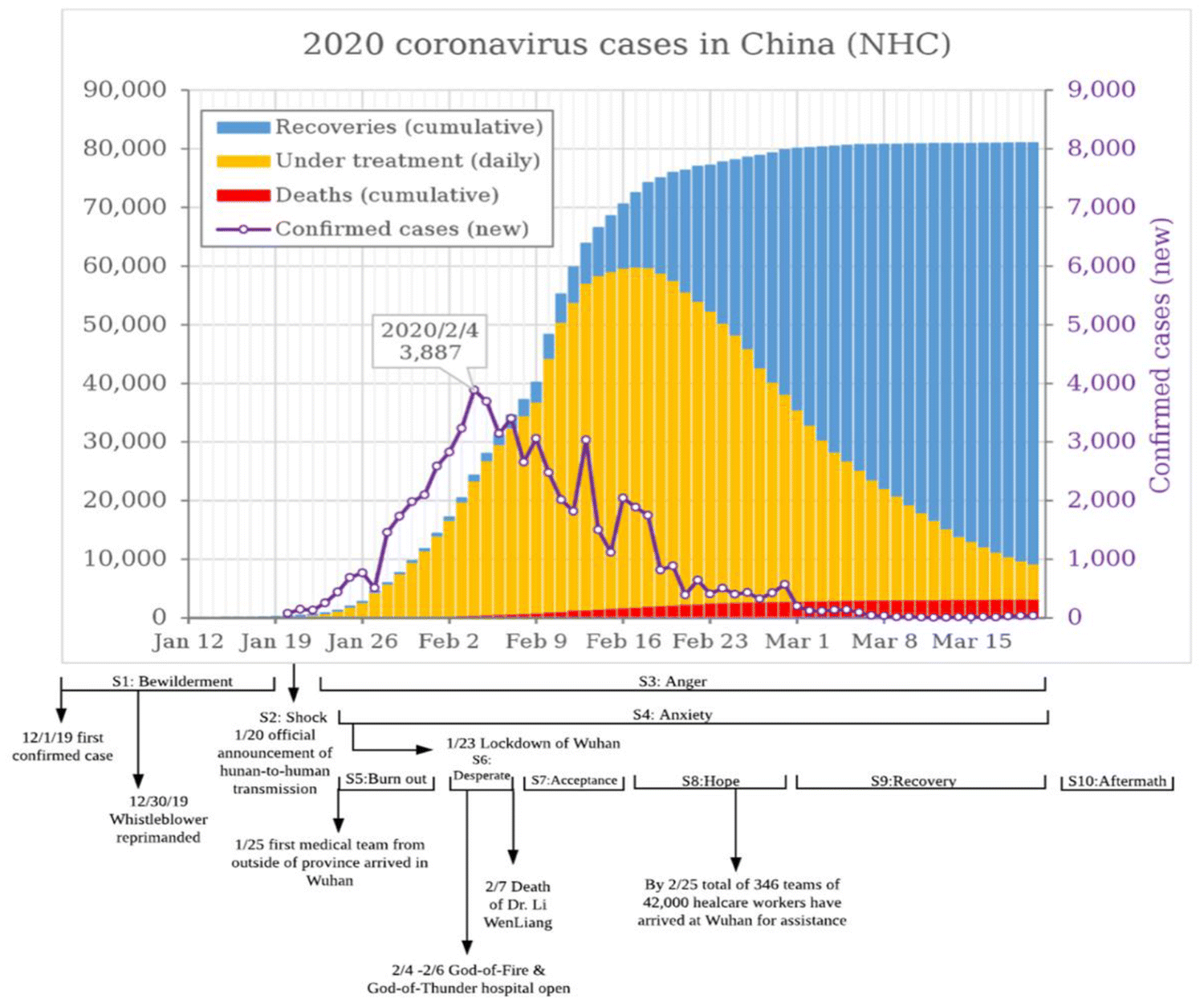
This was a unique experience. First, this crisis has lasted for months in China and continued to progress globally. This is unlike the other crises such as earthquake or volcano eruption, which last for shorter periods of time and leaving people to deal primarily with the aftermath. Therefore, people are exposed to continuous loss and trauma for a long period of time. Second, our approach was novel. There is little research on the use of social media for crisis intervention, despite the growing popularity of social media among all age groups. A PubMed search using key word “crisis intervention” and “social media” only found one article (Bailey et al. 2018). Although there are quite few very recently published articles discussing the mental health consequences of COVID-19 for both general public (Dong et al. 2020; Wang et al. 2020; Li et al. 2020; Ho et al. 2020) and healthcare personnel (Lai et al. 2020; Chen et al. 2020), including other online mental health services or telehealth approaches in China (Liu et al. 2020; Zhou et al. 2020), but our practice model is unique. Finally, this was a grassroots international effort comprised of volunteers. This demonstrates the value of peer support, even when the peers are fellow professionals.
Although we did not collect formal outcome data, and the results can only be considered anecdotal, there is some evidence indicating this might be a helpful intervention. The total number of the counseling group was stable at around 300 members throughout the whole course of the project. To our knowledge, this is the largest and most stable group of its kind in the country. Preliminary review suggests that many of those served found the intervention helpful.
Our experience has its limitation. First, the situation in China is unique. The outcome is influenced by the Chinese political and social infrastructure and cultural beliefs. While the central government was able to eventually mobilize and re-distribute a great number of healthcare professionals to support Wuhan, its censorship had a noticeable impact on the healthcare professionals, social media peer support group, and the particular modality of our intervention.
Culture was another factor. Traditional Chinese culture tends to value collectivism, and self-sacrificing for the society’s good and dismisses emotional expression. This created more difficulty for engagement, especially at the beginning of our work. Furthermore, some of the topics raised in the chats were not considered appropriate for various of reasons, such as religious ones. The difference in time zones was also a barrier.
The World Health Organization declared Coronavirus as global pandemic on March 11, 2020. Many countries eventually had various degrees of lockdown. Hence, we believe that healthcare workers elsewhere would experience the similar mental health crises. The degree of impact will vary according each region or country’s unique situation; therefore, we believe development of interventional strategies based on local experience might be needed.
Several important lessons were learned from this experience. First, was that “do no harm” was the top priority. We needed to consider both clinical and non-clinical factors to ensure we were providing help not harm. We found that stage 3/4 might be the best time point to intervene, as earlier, HCPs might not have the need, but later, HCPs already have experienced significant impairment. Social media provided easy accessibility, and anonymity to HCPs, it reduced barriers and resistance and improved engagement. But, the clinical skill we utilize during routine work, such as interviewing and psychotherapy techniques, were not directly applied to this setting without adjustment and flexibility.
In summary, our group mobilized quickly in response to the COVID-19 epidemic in Wuhan, China. We organized a group of active clinical mental health providers who were familiar with Chinese culture and were willing to voluntarily provide crisis peer-to-peer psychological support to the frontline healthcare providers in Wuhan. We utilized an existing social media platform. We found that it was, despite many challenges, an effective way to implement mental health support. This form of disaster outreach via social media requires further study for development and improvement in different settings. Nevertheless, in the time of COVID-19 pandemic, psychological support to the frontline responders and community is of paramount importance. Thus, we hope our work can shed some lights on effective mental health disaster outreach utilizing existing cyber technology to help workers fighting this unprecedented pandemic.
Bailey, E., et al. (2018). Theoretical and empirical foundations of a novel online social networking intervention for youth suicide prevention: A conceptual review. Journal of Affective Disorders,238, 499–505. https://doi.org/10.1016/j.jad.2018.06.028.
Chen, Q., et al. (2020). Mental health care for medical staff in China during the COVID-19 outbreak. Lancet Psychiatry,7(4), e15–e16. https://doi.org/10.1016/S2215-0366(20)30078-X.
Dong, L., et al. (2020). Public mental health crisis during COVID-19 Pandemic, China. Emerging Infectious Diseases. https://doi.org/10.3201/eid2607.200407.
Ho, C. S., et al. (2020). Mental health strategies to combat the psychological impact of COVID-19 beyond paranoia and panic. Annals of the Academy of Medicine, Singapore,49(1), 1–3.
Lai, J., et al. (2020). Factors associated with mental health outcomes among health care workers exposed to coronavirus disease 2019. JAMA Network Open,3(3), e203976. https://doi.org/10.1001/jamanetworkopen.2020.3976.
Li, Z., et al. (2020). Vicarious traumatization in the general public, members, and non-members of medical teams aiding in COVID-19 control. Brain, Behavior, and Immunity. https://doi.org/10.1016/j.bbi.2020.03.007.
Liu, S., et al. (2020). Online mental health services in China during the COVID-19 outbreak. Lancet Psychiatry,7(4), e17–e18. https://doi.org/10.1016/S2215-0366(20)30077-8.
Maunder, R. G., et al. (2006). Long-term psychological and occupational effects of providing hospital healthcare during SARS outbreak. Emerging Infectious Diseases,12(12), 1924–1932.
Wang, C., et al. (2020). Immediate psychological responses and associated factors during the initial stage of the 2019 Coronavirus Disease (COVID-19) epidemic among the general population in China. International Journal of Environmental Research and Public Health. https://doi.org/10.3390/ijerph17051729.
Zhou, X., et al. (2020). The role of telehealth in reducing the mental health burden from COVID-19. Telemedicine and e-Health. https://doi.org/10.1089/tmj.2020.0068.
List of group members with professional credential based on the time of joining: Pu Cheng, Psychiatrist, IN, Qi Ling, Psychiatrist, NY, Yong-Tong Li, Psychiatrist, PA, Peng Pang, Psychiatrist, NY, Bo Wu, Psychiatrist, TX, Junyong Jia, Psychiatrist, MD, Xiaocheng Dai, AMFT, CA, Liang Bao, Psychologist, Canada, Yanye Maggie Li, LPC, PA, Jinghan Wang, MSW, NY, Pan Li, Therapist, MA, Ke Liu, LPC, MI, Wenting Kang, LCPC, IL, Xiaojin Lin, LCSW/MSW, MA, Ge Li, LMSW, TX, Junhua Wang, Psychiatrist, TX, Qingmin Ruan, Psychiatrist, TX, Guohua Xia, Psychiatrist, CA, Xiaonan Liao, MHC, NY, Ci Ma, Psychiatrist, CA, Mei Wang, Psychologist, OH, Yonghong Tan, Psychiatrist, CT, Feng Liu, Psychiatrist, NY, Hong Chai, Psychiatrist, TX, Qingyang Xu, LMSW, NY, Huiyi Chen, LPC, IL, Rou Zhang, LMHC, NY, Yanqing Teng, Therapist, Canada, Xiaoting Bi, LPC, PA, Zhihong Guo, Psychiatrist, MD, Lu Liu, MSW, CA, Xiaoli Wang, LPC, TX, Xueling Fu, Psychiatrist, TX, Hong Wang, RN, Australia, Esther Zhang, LMHC, WA, Yueheng Han, Psychiatrist, PA, Yunyun Lu, RN, WA, Xiaohui Zhang, Psychiatrist, PA, Fang Yang, Psychiatrist, TX, Xiaoying Chang, Psychiatrist, NY, Yu Quan, Psychiatrist, TX, Yongyao Chen, Psychiatrist, NC, Shumin Zhang, Psychiatrist, MA, Wei Jiang, Psychiatrist/Internist, NC, Liren Li, Psychiatrist, NJ. Special appreciation to Dr. Kay Levine for your professional help and instruction.